Type 1 diabetes: Causes and development
Scientific support: Prof. Dr. Carolin Daniel, Dr. Martin Scherm
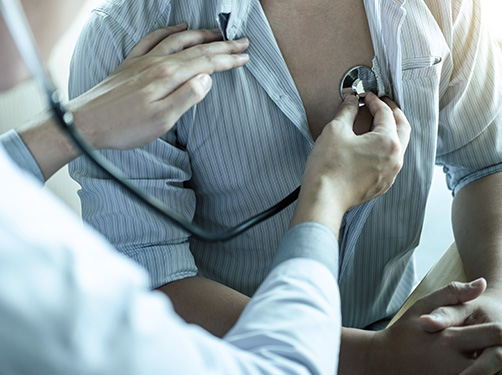
In type 1 diabetes, the body's own immune system attacks the beta cells in the pancreas. These beta cells produce insulin. As more and more beta cells are destroyed and the body releases less insulin into the blood, blood sugar rises and type 1 diabetes develops.
Basically, any person can develop type 1 diabetes. However, the risk of developing the autoimmune disease increases if a close relative, e.g., mother or father, has type 1 diabetes.
The causes of type 1 diabetes are not yet fully understood. In addition to genetic predisposition, environmental factors are suspected to trigger type 1 diabetes in early childhood. If viral diseases occur in the first years of life, subsequent onset of type 1 diabetes seems more likely. The gut microbiome and nutrition in infancy are also discussed as risk factors.
If certain antibodies are detected in the blood, it is highly likely that type 1 diabetes will be diagnosed in the following years.
Contents
1. Is type 1 diabetes hereditary?
Type 1 diabetes or predisposition for type 1 diabetes can be inherited from close relatives. If the genetic risk is increased because one’s mother, father, brother or sister has type 1 diabetes, 10 out of 100 people will develop type 1 diabetes. Children with fathers who have type 1 diabetes are at a higher risk of developing the autoimmune disease than children with mothers who have type 1 diabetes.
- 3 out of 100 children whose mother has type 1 diabetes will also develop the disease.
- 5 out of 100 children whose father has type 1 diabetes also develop type 1 diabetes.
- If one parent and one sibling have type 1 diabetes, 8 out of 100 children will develop the disease.
- If 2 close relatives have type 1 diabetes (for example, both parents), 25 out of 100 children develop diabetes.
- In the general population, 3 to 4 out of every 1,000 people currently develop type 1 diabetes.
The increased genetic risk therefore does not mean that type 1 diabetes will always develop if it is inherited. In 90 out of 100 children newly diagnosed with type 1 diabetes, the disease does not previously occur in the family. Therefore, it is said that any child may be at risk of developing type 1 diabetes.
The risk of developing type 1 diabetes is particularly increased in childhood and early adulthood. If islet autoimmunity does not occur during this time, the likelihood of developing type 1 diabetes at a later point decreases from year to year.
Studies have shown that many different genes are involved in the development of type 1 diabetes. However, the factors leading to the development of the disease have not been specifically identified.
Good to know:
Type 1 diabetes is on the rise worldwide. Overall disease rates are expected to double by 2040.
2. Which environmental factors promote type 1 diabetes?
In addition to genetic factors, environmental influences play an important role in the development of type 1 diabetes. But it is not yet known exactly which environmental influences these are. There is evidence that viral infections may trigger the autoimmune process. The gut microbiome and nutrition in infants may also play a role. Particularly in individuals at high genetic risk, the first years of life are a vulnerable period in which environmental factors may further increase the risk of developing islet autoimmunity.
The following environmental factors in particular are suspected to increase the risk of developing type 1 diabetes:
- Early infection with coxsackieviruses, which can trigger respiratory diseases in children.
- Infections with rubella or mumps viruses are also suspected of promoting type 1 diabetes. The viruses can damage the cells in the pancreas that produce insulin.
- Feeding food containing gluten to infants before they are 4 months old also appears to increase the risk of type 1 diabetes. Gluten is a specific protein in cereals and is found in bakery products or food made of wheat, spelt, oats, rye, barley and other types of cereals.
- There is evidence that vitamin D deficiency and lack of sun exposure are associated with an increased risk of developing type 1 diabetes.
- Birth by C-section in children who are genetically predisposed also appears to increase the risk of actually developing type 1 diabetes.
- Presumably, the composition of the intestinal flora also has an influence on the development of type 1 diabetes.
Because an unusually high number of new cases of type 1 diabetes have occurred since the onset of the coronavirus pandemic, an interrelationship between infection with the SARS-CoV-2 virus and the onset of type 1 diabetes is also being examined. However, studies suggest that the increase in new cases is more likely due to indirect consequences of the pandemic as well as other environmental influences.
Whether early feeding of cow’s milk protein increases the risk of type 1 diabetes is still debated: While some studies support this assumption, others have found no increased risk. The same applies to the duration of breastfeeding of infants; here, too, studies show different results. Overall, however, longer breastfeeding duration appears to reduce the risk of type 1 diabetes.
3. Development of type 1 diabetes
The autoimmune disease type 1 diabetes ultimately destroys the beta cells in the pancreas. As a result, the beta cells do not produce enough insulin and are eventually no longer able to produce insulin at all. Therefore, sugar – and thus important energy for the body – can no longer be released from the blood and supplied into the cells of the organs. Therefore, the blood sugar level rises. Insulin must then be injected to provide the body with the vital hormone.
The beta cells that produce insulin are grouped in certain areas of the pancreas, known as the islets of Langerhans. This is why they are also called islet cells.
The role of antibodies
Antibodies are tools of the immune system. They mark foreign substances, such as pathogens like bacteria or viruses, to prepare for them to be destroyed by immune cells.
With an autoimmune disease, the immune system is no longer able to properly distinguish between friend and foe. Then autoantibodies (Greek, auto = self) and corresponding immune cells attack the body’s own cells and thus trigger inflammation. With type 1 diabetes, this then destroys the islet cells. The responsible antibodies are called islet auto-antibodies.
Antibodies in type 1 diabetes
Years before diabetes develops, antibodies against certain parts of the beta cells or insulin itself can be identified. Type 1 diabetes is diagnosed when 2 or more of these autoantibodies are detected.
Autoantibodies found in type 1 diabetes include:
- Islet Cell Antibodies (ICA)
- Insulin autoantibodies (IAA)
- Glutamate decarboxylase antibodies (GADA)
- Tyrosine phosphatase antibodies IA-2- (IA2A)
- Zinc transporter 8 antibodies (ZnT-8A)
In approximately 5 percent of people with type 1 diabetes, autoantibodies cannot be detected. In this case, experts speak of antibody-negative type 1 diabetes.
Good to know:
Symptoms of high blood sugar levels which in turn indicate type 1 diabetes include:
- constant feeling of thirst
- frequent urination
- excessive fatigue
- weight loss
If such signs are detected, a doctor should be contacted as soon as possible.
Other possible signs of type 1 diabetes – which are, however, also seen in other diseases – include nocturnal wetting, nausea, vomiting, weakness, frequent urinary tract infections, or a drop in one’s performance.
In an infant, signs of type 1 diabetes (rapid breathing, fatigue, sleepiness, vomiting, diarrhea, body fluid deficit) should be taken seriously, even if they are difficult to distinguish from another disease.
Stages in the development of diabetes
The attacks of the immune system against beta cells in the early phase of the development of type 1 diabetes last months to years. At the beginning there are no symptoms. Doctors cannot find anything abnormal during routine examinations either. They tend to measure fasting blood sugar levels. This does not increase until about 80 percent of the beta cells are destroyed and no longer produce insulin. Such a blood glucose test therefore only gives an indication at a later stage that there is damage to the insulin-producing islet or beta cells.
Experts classify type 1 diabetes as having 3 stages:
- Stage 1: At least 2 characteristic autoantibodies are detected in the blood. People do not have any symptoms or abnormal metabolic readings. So blood sugar levels are not elevated.
- Stage 2: The increasing destruction of the insulin-producing beta cells is having an ever-increasing effect on blood glucose metabolism: Since the body produces too little insulin, blood sugar levels rise. However, there are usually no symptoms at this stage.
- Stage 3: Due to the pronounced insulin deficiency, the persons affected show typical symptoms such as excessive thirst, frequent urination, fatigue or weight loss. The clinical picture of type 1 diabetes is full-blown and insulin must be injected.
Remission phase (“honeymoon phase”)
Shortly after starting insulin therapy for type 1 diabetes, a remission phase may occur, which is also known as “honeymoon phase.” In this phase, the metabolic situation improves for a short time. The beta cells produce small amounts of insulin again. Persons affected need to inject only a small amount of insulin or none at all. This remission phase lasts a few months to years until the beta cells are completely depleted and no longer produce insulin, and insulin must be injected again. A longer remission phase in type 1 diabetes is assumed to be associated with a better long-term prognosis and a lower risk of type 1 diabetes complications.
Note: The duration of the phases in the development of type 1 diabetes differs from individual to individual.
4. Early detection of type 1 diabetes is possible
A gene test can be used to determine if an infant is at risk of developing type 1 diabetes. The test can be performed free of charge throughout Germany as part of the Freder1k study in babies whose parents or siblings have type 1 diabetes. In the states of Bavaria, Saxony, Thuringia, and Lower Saxony, screening is possible without close relatives having the autoimmune disease. All that is needed is a few drops of blood, for example from the newborn's heel.
Learn more about the Freder1k study and newborn screening here (Link in German)
Children and adolescents between 1 and 21 years of age can also be tested for the presence of islet autoantibodies as part of the Fr1da study. Screening is available throughout Germany for relatives of people with type 1 diabetes. If there is no known family history of diabetes, children between 2 and 10 years of age can be tested free of charge in Bavaria, Saxony, Lower Saxony, and Hamburg.
Learn more about early detection examinations (Link in German)
If no abnormalities are found during type 1 diabetes risk screening, it is very unlikely that type 1 diabetes will develop at a later point. However, if an increased risk of type 1 diabetes is detected early, good treatment and care from the beginning can help prevent dangerous metabolic problems.
Current studies on the prevention of type 1 diabetes
Genetic testing or the detection of specific autoantibodies offer the possibility of early identifying children with an increased risk of developing type 1 diabetes. There are several ongoing clinical studies based on these early detection options. These aim to prevent the disease from developing in often very young children who are at risk.
Current research approaches to preventing type 1 diabetes are, for example, engaged in
- the use of active substances for the preservation of beta cell function;
- a positive influence of certain probiotics on the intestinal flora;
- the administration of insulin powder with food, and other approaches.
Good to know:
In the majority of cases, type 1 diabetes is diagnosed in children under the age of 14. In Germany, about 3,700 children and adolescents contract the autoimmune disease every year. Boys are affected more often than girls.
Diabetes can also occur in newborns, although rarely only.
Sometimes the persons affected do not develop type 1 diabetes until adulthood. This autoimmune-related diabetes with its delayed onset in adults is known as LADA diabetes. In the majority of cases, the persons affected are older than 30 years and laboratory tests reveal at least one autoantibody in the blood that attacks the structures of the pancreas.
Sources:
Achenbach, P.: Risiko für Typ-1-Diabetes auch bei Nachkommen erhöht? In: MMW Fortschritte der Medizin, 2022, 164: 67-69
Beyerlein, A. et al.: Infections in Early Life and Development of Type 1 Diabetes. In: JAMA, 2016, 315: 1899-1901
Bonifacio, E. et al.: Predicting type 1 diabetes using biomarkers. In: Diabetes Care, 2015, 38: 989-996
Buzzetti, R. et al.: Adult-onset autoimmune diabetes. In: Nat Rev Dis Primers, 2022, 8: 63
Chmiel, R. et al.: Early infant feeding and risk of developing islet autoimmunity and type 1 diabetes. In: Acta Diabetol, 2015, 52: 621-624
Del Chierico, F. et al.: Pathophysiology of Type 1 Diabetes and Gut Microbiota Role. In: Int J Mol Sci, 2022, 23: 14650
Deutsche Diabetes Gesellschaft (DDG): S3-Leitlinie Therapie des Typ-1-Diabetes. 2. Auflage. 2018
DiMeglio, L. A. et al.: Type 1 diabetes. In: Lancet, 2018, 391: 2449-2462
Fr1da plus: Typ-1-Diabetes: Früh erkennen – Früh gut behandeln. (Letzter Abruf: 16.05.2023)
GPPAD: Freder1k-Studie. Ein erhöhtes Typ-1-Diabetesrisiko früh erkennen und vorbeugend handeln. (Letzter Abruf: 16.05.2023)
Gregory, G. A. et al.: Global incidence, prevalence, and mortality of type 1 diabetes in 2021 with projection to 2040: a modelling study. In: Lancet Diabetes Endocrinol, 2022, 10: 741-760
Insel, R. A. et al.: Staging presymptomatic type 1 diabetes: a scientific statement of JDRF, the Endocrine Society, and the American Diabetes Association. In: Diabetes Care, 2015, 38: 1964-1974
Kamrath, C. et al.: Incidence of Type 1 Diabetes in Children and Adolescents During the COVID-19 Pandemic in Germany: Results From the DPV Registry. In: Diabetes Care, 2022 (online)
Knip, M. et al.: Effect of Hydrolyzed Infant Formula vs Conventional Formula on Risk of Type 1 Diabetes: The TRIGR Randomized Clinical Trial. In: JAMA, 2018, 319: 38-48
Lampousi, A. M. et al.: Dietary factors and risk of islet autoimmunity and type 1 diabetes: a systematic review and meta-analysis. In: EbioMedicine, 2021, 72: 103633
Norris, J. M. et al.: Timing of Initial Cereal Exposure in Infancy and Risk of Islet Autoimmunity. In: JAMA, 2003, 290: 1713-1720
Parkkola, A. et al.: Extended Family History of Type 1 Diabetes and Phenotype and Genotype of Newly Diagnosed Children. In: Diabetes Care, 2013, 36: 348-354
Rewers, M. et al.: The Environmental Determinants of Diabetes in the Young (TEDDY) Study: 2018 Update. In: Curr Diab Rep, 2018, 18: 136
Robert Koch-Institut. Diabetes in Deutschland - Kinder und Jugendliche. Inzidenz Typ-1-Diabetes. (Letzter Abruf: 16.05.2023)
Robert Koch-Institut: Diabetes Surveillance. (Letzter Abruf: 16.05.2023)
Sims, E. K. et al.: Screening for Type 1 Diabetes in the General Population: A Status Report and Perspective. In: Diabetes, 2022, 71: 610-623
Zhong, T. et al.: The remission phase in type 1 diabetes: Changing epidemiology, definitions, and emerging immuno-metabolic mechanisms. In: Diabetes Metab Res Rev, 2020, e3207
Ziegler, A. G. et al.: Primary prevention of beta-cell autoimmunity and type 1 diabetes – The Global Platform for the Prevention of Autoimmune Diabetes (GPPAD) perspectives. In: Mol Metab, 2016, 5: 255-262
Ziegler, A. G. et al.: Seroconversion to Multiple Islet Autoantibodies and Risk of Progression to Diabetes in Children. In: JAMA, 2013, 309: 2473-2479
Zorena, K. et al.: Environmental Factors and the Risk of Developing Type 1 Diabetes-Old Disease and New Data. In: Biology, 2022, 11: 608
As of: 16.05.2023